A Two-Part Series On Traumatic Brain Injuries (Part 2)
Emergency Management of Traumatic Brain Injury
Mild traumatic brain injuries do not often require treatment, with patient fully recovering after the injury. However, the person who has suffered mild TBI should be closely monitored. If the initial symptoms persist or worsen, or new symptoms develop, the person should be brought back to the emergency department for medical attention.
On the other hand, moderate to severe traumatic brain injuries often happen as an emergency and since they can lead to serious consequences, doctors and first responders must assess the situation immediately.
Emergency care for brain trauma focuses on ensuring an adequate airway and blood supply and preventing further injury. People who suffered TBI may also have other injuries that require immediate attention.
If you are at the scene of the accident or arrived immediately after the injury, it is important that you contact your local emergency service immediately. Do not attempt to move the injured person as it can cause more harm than good. It is also important to take note of information which the first aider or emergency personnel may find useful, such as:
- how the injury occurred,
- did the victim lose consciousness and for how long,
- what parts of the body or head was injured,
- what type of object hit the person,
- how forceful the impact was.
The information that bystanders and witnesses provide may be helpful in assessing the severity of the injury and determining the type of injury that might have been sustained.
The first aider assesses the consciousness of the victim using the Glasgow Coma Scale. This is a 15-point test used to assess the initial severity of the injury. In this test, the person is made to follow directions and move their limbs and eyes. Speech and response to stimuli provide crucial clues to the neurologic state of the patient. Although higher scores indicate mild injury, it does not guarantee the prognosis of the victim. Check out the video below for more information about using the Glasgow Coma Scale.
The patient is carefully transferred and transported to the nearest emergency facility for further examination. Once in the emergency department, the focus is on preventing secondary damage caused by bleeding, inflammation or lack of oxygen in the brain.
How is TBI Diagnosed?
There are many different tests that are used to diagnose the location and extent of the injury. Imaging tests such as Magnetic Resonance Imaging (MRI) and Computerized Tomography (CT) are some of the initial diagnostic
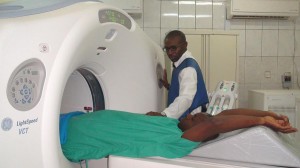
tests done. These tests provide visualization of the internal structures of the brain allowing detection of blood clots, bleeding, swelling or bruising of the brain tissues.
In case of closed head injuries that cause increased pressure inside the skull, the doctor may recommend intra-cranial pressure monitoring. A probe is inserted into the skull to monitor pressure inside.
How is TBI treated?
The treatment of TBIs often include use of medications, particularly diuretics to reduce inflammation of brain tissue, anti-seizure drugs to avoid additional damage to brain caused by a seizure, and coma-inducing drugs to minimize the brain’s demand for oxygen.
Surgery may also be recommended to remove hematomas, to repair fractured skull, or to open up a small slit in the skull for drainage of accumulated fluids or provide additional space for swollen tissue.
The treatment does not end with hospitalization. Most people who have suffered moderate to severe brain injury require long term rehabilitation to improve abilities that may have been affected. The support of loved ones and significant others is crucial throughout the treatment and rehabilitation process.
I was wondering if you ever thought of changing the page layout of your site? Its very well written; I love what youve got to say. But maybe you could a little more in the way of content so people could connect with it better. Youve got an awful lot of text for only having one or 2 images. Maybe you could space it out better?